This year’s predictions on the biopharma financing and funding environment are more optimistic than they were last year, with the persistent caveat of macroeconomic uncertainty, plus unresolved litigation on policy issues such as the Inflation Reduction Act. With deal activity increasing and the promise of novel product approvals in key therapeutic areas next year, however, small biotechs and (some) Big Pharmas appear poised to steer the industry into calmer waters. Business model creativity will become increasingly mandatory for companies marketing expensive products for small patient populations and larger population drugs in categories like obesity and CNS disorders.
Author: Staff
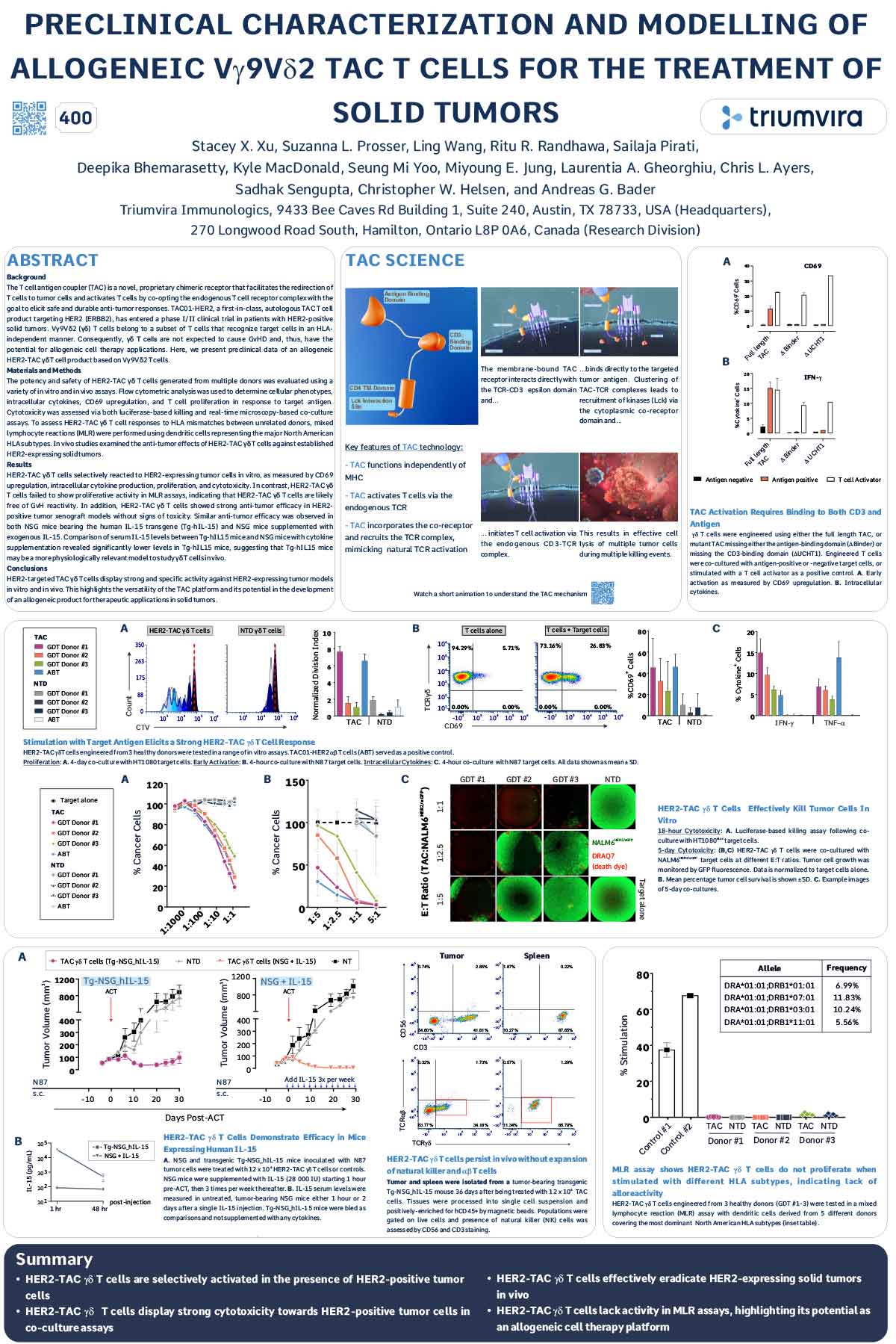
Preclinical Characterization and Modeling of Allogeneic Vγ9Vδ2 TAC T Cells for the Treatment of Solid Tumors
ABSTRACT
Background
The T cell antigen coupler (TAC) is a novel, proprietary chimeric receptor that facilitates the redirection of T cells to tumor cells and activates T cells by co-opting the endogenous T cell receptor complex with the goal to elicit safe and durable anti-tumor responses. TAC01-HER2, a first-in-class, autologous TAC T cell product targeting HER2 (ERBB2), has entered a phase I/II clinical trial in patients with HER2-positive solid tumors. Vγ9Vδ2 (γδ) T cells belong to a subset of T cells that recognize target cells in an HLAindependent manner. Consequently, γδ T cells are not expected to cause GvHD and, thus, have the potential for allogeneic cell therapy applications. Here, we present preclinical data of an allogeneic HER2-TAC γδ T cell product based on Vγ9Vδ2 T cells.
Materials and Methods
The potency and safety of HER2-TAC γδ T cells generated from multiple donors was evaluated using a variety of in vitro and in vivo assays. Flow cytometric analysis was used to determine cellular phenotypes, intracellular cytokines, CD69 upregulation, and T cell proliferation in response to target antigen. Cytotoxicity was assessed via both luciferase-based killing and real-time microscopy-based co-culture assays. To assess HER2-TAC γδ T cell responses to HLA mismatches between unrelated donors, mixed lymphocyte reactions (MLR) were performed using dendritic cells representing the major North American HLA subtypes. In vivo studies examined the anti-tumor effects of HER2-TAC γδ T cells against established HER2-expressing solid tumors.
Results
HER2-TAC γδ T cells selectively reacted to HER2-expressing tumor cells in vitro, as measured by CD69 upregulation, intracellular cytokine production, proliferation, and cytotoxicity. In contrast, HER2-TAC γδ T cells failed to show proliferative activity in MLR assays, indicating that HER2-TAC γδ T cells are likely free of GvH reactivity. In addition, HER2-TAC γδ T cells showed strong anti-tumor efficacy in HER2- positive tumor xenograft models without signs of toxicity. Similar anti-tumor efficacy was observed in both NSG mice bearing the human IL-15 transgene (Tg-hIL-15) and NSG mice supplemented with exogenous IL-15. Comparison of serum IL-15 levels between Tg-hIL15 mice and NSG mice with cytokine supplementation revealed significantly lower levels in Tg-hIL15 mice, suggesting that Tg-hIL15 mice may be a more physiologically relevant model to study γδ T cells in vivo.
Conclusions
HER2-targeted TAC γδ T cells display strong and specific activity against HER2-expressing tumor models in vitro and in vivo. This highlights the versatility of the TAC platform and its potential in the development of an allogeneic product for therapeutic applications in solid tumors.
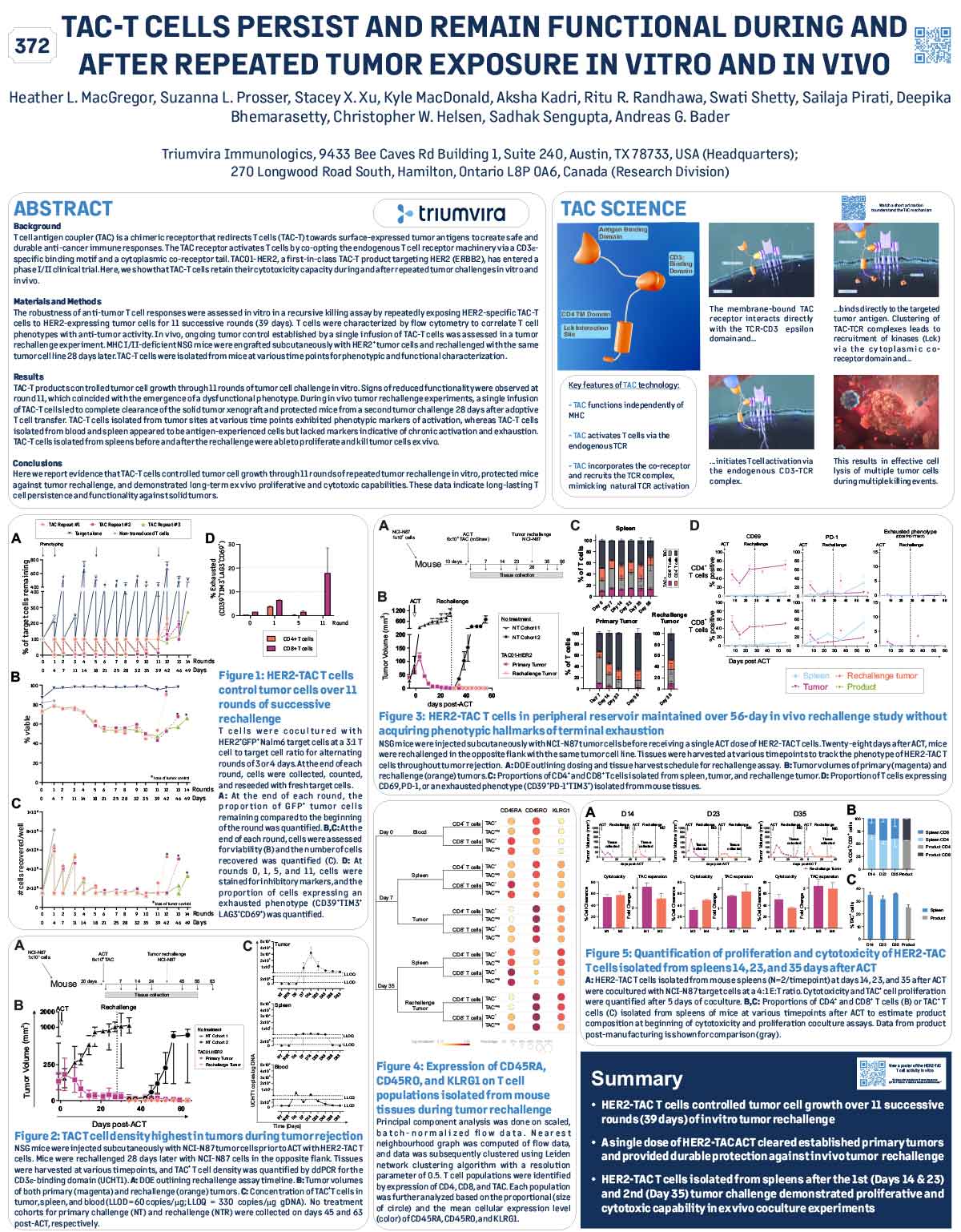
TAC-T Cells Persist and Remain Functional During and After Repeated Tumor Exposure In Vitor and In Vivo
ABSTRACT
Background
T cell antigen coupler (TAC) is a chimeric receptor that redirects T cells (TAC-T) towards surface-expressed tumor antigens to create safe and durable anti-cancer immune responses. The TAC receptor activates T cells by co-opting the endogenous T cell receptor machinery via a CD3e-specific binding motif and a cytoplasmic co-receptor tail. TAC01-HER2, a first-in-class TAC-T product targeting HER2 (ERBB2), has entered a phase I/II clinical trial. Here, we show that TAC-T cells retain their cytotoxicity capacity during and after repeated tumor challenges in vitro and in vivo.
Materials and Methods
The robustness of anti-tumor T cell responses were assessed in vitro in a recursive killing assay by repeatedly exposing HER2-specific TAC-T cells to HER2-expressing tumor cells for 11 successive rounds (39 days). T cells were characterized by flow cytometry to correlate T cell phenotypes with anti-tumor activity. In vivo, ongoing tumor control established by a single infusion of TAC-T cells was assessed in a tumor rechallenge experiment. MHC I/II-deficient NSG mice were engrafted subcutaneously with HER2+ tumor cells and rechallenged with the same tumor cell line 28 days later. TAC-T cells were isolated from mice at various time points for phenotypic and functional characterization.
Results
TAC-T products controlled tumor cell growth through 11 rounds of tumor cell challenge in vitro. Signs of reduced functionality were observed at round 11, which coincided with the emergence of a dysfunctional phenotype. During in vivo tumor rechallenge experiments, a single infusion of TAC-T cells led to complete clearance of the solid tumor xenograft and protected mice from a second tumor challenge 28 days after adoptive T cell transfer. TAC-T cells isolated from tumor sites at various time points exhibited phenotypic markers of activation, whereas TAC-T cells isolated from blood and spleen appeared to be antigen-experienced cells but lacked markers indicative of chronic activation and exhaustion. TAC-T cells isolated from spleens before and after the rechallenge were able to proliferate and kill tumor cells ex vivo.
Conclusions
Here we report evidence that TAC-T cells controlled tumor cell growth through 11 rounds of repeated tumor rechallenge in vitro, protected mice against tumor rechallenge, and demonstrated long-term ex vivo proliferative and cytotoxic capabilities. These data indicate long-lasting T cell persistence and functionality against solid tumors.
A Phase 1/2 Study Investigating the Safety and Efficacy of Autologous TAC T Cells in Subjects with Unresectable, Locally Advanced or Metastatic CLDN18.2+ Solid Tumors
INTRODUCTION
• The T cell antigen coupler (TAC) is a novel, proprietary chimeric receptor that facilitates the re-direction of T cells to tumor
cells and activates T cells by co-opting the endogenous T cell receptor complex, with the goal of eliciting a safe and durable antitumor
response. In preclinical models, TAC-engineered T cells effectively eradicate tumor cells in vitro and in vivo without
toxicities typically associated with engineered T cell products. TAC01-CLDN18.2 is an autologous T cell product comprising T
cells expressing the CLDN18.2 TAC, which specifically recognizes CLDN18.2+ cells.
• TACTIC-3 (NCT05862324) is an open-label, multicenter phase I/II study that aims to establish safety, maximum tolerated dose
(MTD), recommended phase 2 dose (RP2D), pharmacokinetic profile, and efficacy of TAC01-CLDN18.2 in patients with
CLDN18.2 positive, HER2-negative solid tumors by immunohistochemistry (i.e. gastric, GEJ, esophageal adenocarcinoma,
PDAC, colorectal cancer, cholangiocarcinoma, ovarian mucinous cancer, gallbladder cancer, and NSCLC) who have measurable
disease after at least 2 prior anti-cancer therapies.
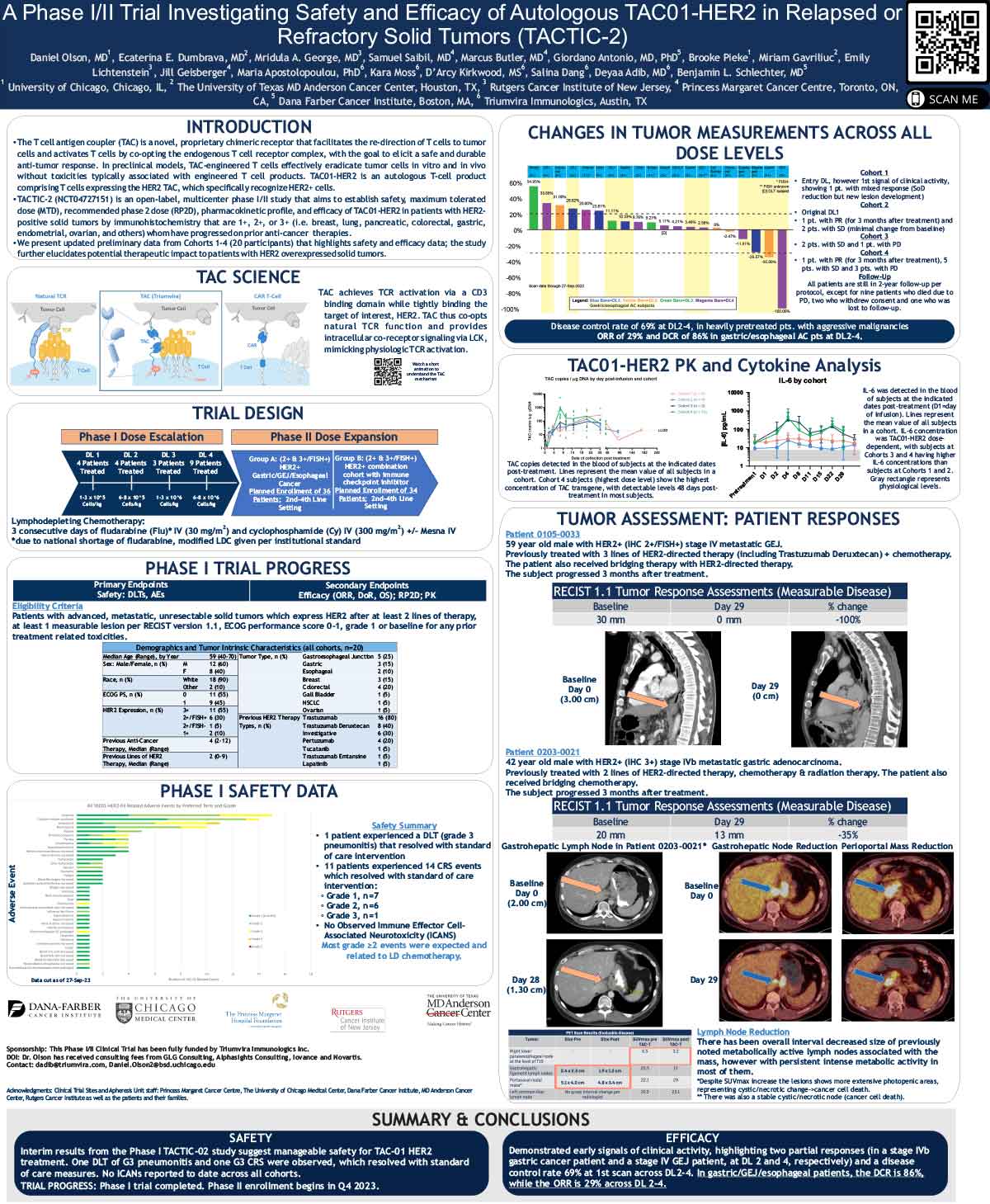
A Phase I/II Trial Investigating Safety and Efficacy of Autologous TAC01-HER2 in Relapsed or Refractory Solid Tumors (TACTIC-2)
INTRODUCTION
• The T cell antigen coupler (TAC) is a novel, proprietary chimeric receptor that facilitates the re-direction of T cells to tumor
cells and activates T cells by co-opting the endogenous T cell receptor complex, with the goal of eliciting a safe and durable
anti-tumor response. In preclinical models, TAC-engineered T cells effectively eradicate tumor cells in vitro and in vivo
without toxicities typically associated with engineered T cell products. TAC01-HER2 is an autologous T-cell product
comprising T cells expressing the HER2 TAC, which specifically recognizes HER2+ cells.
• TACTIC-2 (NCT04727151) is an open-label, multicenter phase I/II study that aims to establish safety, maximum tolerated
dose (MTD), recommended phase 2 dose (RP2D), pharmacokinetic profile, and efficacy of TAC01-HER2 in patients with HER2-
positive solid tumors by immunohistochemistry that are 1+, 2+, or 3+ (i.e. breast, lung, pancreatic, colorectal, gastric,
endometrial, ovarian, and others) who have progressed on prior anti-cancer therapies.
• We present updated preliminary data from Cohorts 1-4 (20 participants) that highlights safety and efficacy data; the study
further elucidates potential therapeutic impact on patients with HER2 overexpressed solid tumors.
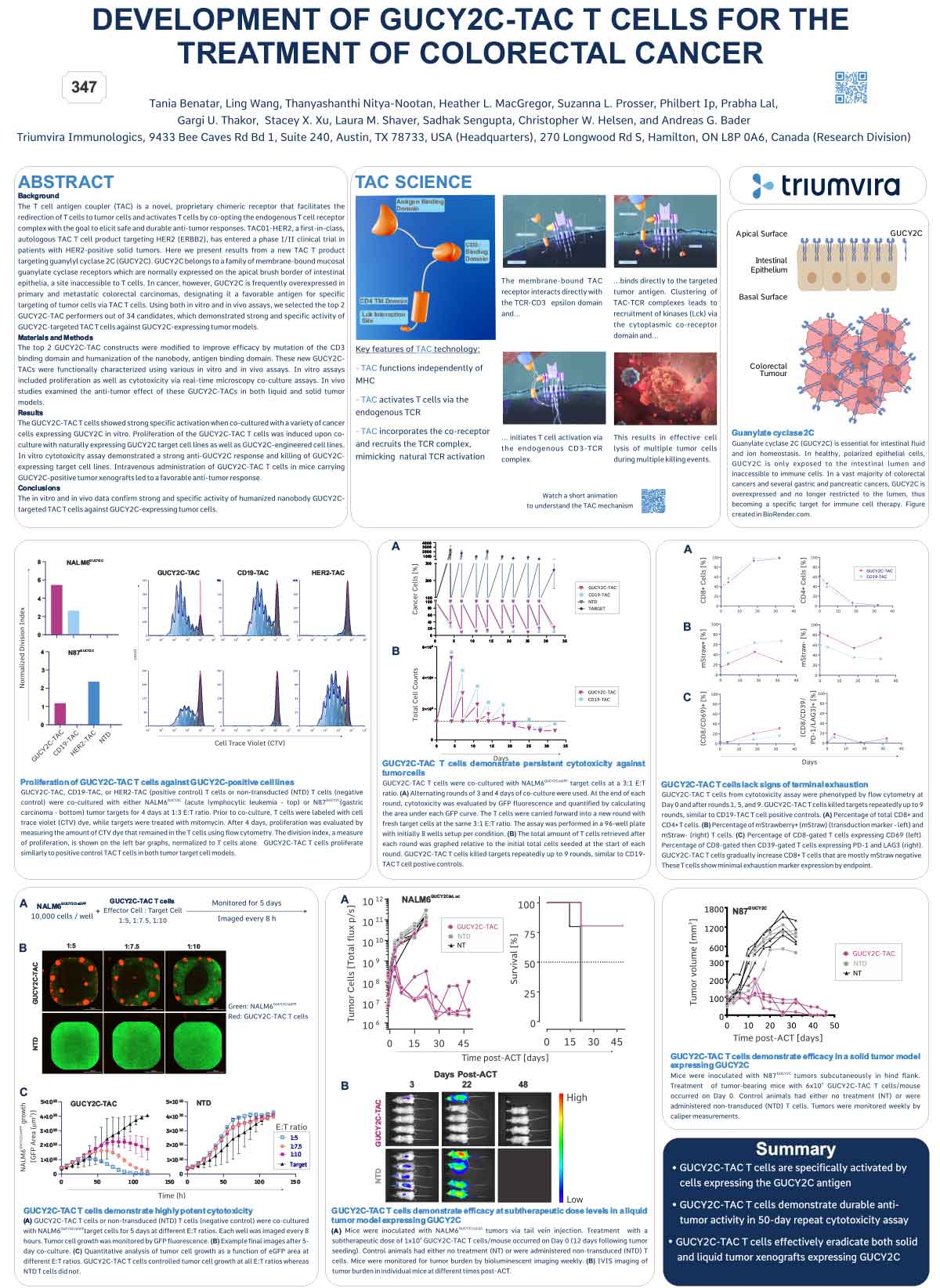
Development of GUCY2C-TAC T Cells for the Treatment of Colorectal Cancer
ABSTRACT
Background
The T cell antigen coupler (TAC) is a novel, proprietary chimeric receptor that facilitates the redirection of T cells to tumor cells and activates T cells by co-opting the endogenous T cell receptor complex with the goal of eliciting safe and durable anti-tumor responses. TAC01-HER2, a first-in-class, autologous TAC T cell product targeting HER2 (ERBB2), has entered a phase I/II clinical trial in patients with HER2-positive solid tumors. Here we present results from a new TAC T product targeting guanylyl cyclase 2C (GUCY2C). GUCY2C belongs to a family of membrane-bound mucosal guanylate cyclase receptors which are normally expressed on the apical brush border of intestinal epithelia, a site inaccessible to T cells. In cancer, however, GUCY2C is frequently overexpressed in primary and metastatic colorectal carcinomas, designating it a favorable antigen for specific targeting of tumor cells via TAC T cells. Using both in vitro and in vivo assays, we selected the top 2 GUCY2C-TAC performers out of 34 candidates, which demonstrated strong and specific activity of GUCY2C-targeted TAC T cells against GUCY2C-expressing tumor models.
Materials and Methods
The top 2 GUCY2C-TAC constructs were modified to improve efficacy by mutation of the CD3 binding domain and humanization of the nanobody, antigen binding domain. These new GUCY2CTACs were functionally characterized using various in vitro and in vivo assays. In vitro assays included proliferation as well as cytotoxicity via real-time microscopy co-culture assays. In vivo studies examined the anti-tumor effect of these GUCY2C-TACs in both liquid and solid tumor models.
Results
The GUCY2C-TAC T cells showed strong specific activation when co-cultured with a variety of cancer cells expressing GUCY2C in vitro. The proliferation of the GUCY2C-TAC T cells was induced upon coculture with naturally expressing GUCY2C target cell lines as well as GUCY2C-engineered cell lines. In vitro, cytotoxicity assay demonstrated a strong anti-GUCY2C response and killing of GUCY2C-expressing target cell lines. Intravenous administration of GUCY2C-TAC T cells in mice carrying GUCY2C-positive tumor xenografts led to a favorable anti-tumor response.
Conclusions
The in vitro and in vivo data confirm the strong and specific activity of humanized nanobody GUCY2C targeted TAC T cells against GUCY2C-expressing tumor cells.
First Patient Dosed in Study of Cell Therapy for Gastric Cancer
Triumvira Immunologics to Present New Clinical and Preclinical Data on its TAC-T Cell Technology at SITC 2023 Annual Meeting
AUSTIN, Texas and HAMILTON, ON and SOUTH SAN FRANCISCO, Calif., Oct. 30, 2023 /PRNewswire/ — Triumvira Immunologics, a clinical-stage company developing novel, targeted autologous and allogeneic T cell therapeutics that co-opt the natural biology of T cells to treat patients with solid tumors, today announced that it will participate with one oral presentation and four posters at the Society for Immunotherapy of Cancer (SITC) 2023 Annual Meeting in San Diego, California, from November 1-5. The company will showcase clinical and preclinical data across various programs, including its ongoing Phase I/II study investigating the safety and efficacy of autologous TAC-T cells targeting human epidermal growth factor receptor 2 (HER2) in relapsed or refractory solid tumors (TACTIC-2 /NCT04727151) and its CLDN18.2, GUCY2C and allogeneic TAC T cell technologies.
TAC01-HER2 is an innovative cell-based therapy that involves the utilization of genetically modified T cells derived from the patient themselves. These cells express a T-cell Antigen Coupler (TAC) which is designed to specifically recognize HER2 in tumors. In addition to the TAC01-HER2 candidate, the company is investigating TAC-GUCY2C for the treatment of colorectal cancer and TAC01-CLDN18.2 for the treatment of pancreatic ductal adenocarcinoma and gastric cancer.
Phase 2 of TACTIC-2 Begins Dosing TAC01-HER2 in HER2+ Gastric/GEJ Cancer
From Targeted Oncology
TAC01-HER2, an autologous TAC-T cell lead asset made to target HER2 in relapsed or refractory gastric and gastroesophageal junction tumors, is being further evaluated in phase 2 of the TACTIC-2 study.
The first patient with relapsed or refractory HER2-positive gastric and gastroesophageal junction (GEJ) tumors has been dosed with TAC01-HER2 in phase 2 of the phase 1/2 TACTIC-2 (NCT04727151) study.1
TAC01-HER2 is an autologous TAC-T cell lead asset being developed to target HER2 in relapsed or refractory gastric and GEJ tumors. The novel cell therapy is based on genetically engineered autologous T cells expressing a T-cell antigen coupler which recognizes HER2.
Triumvira Immunologics Begins Phase II Trial of T-Cell Therapy in HER2-Positive Gastric Cancer
From Precision Medicine Online
NEW YORK – Triumvira Immunologics said on Thursday it had begun treating patients in a Phase II trial of its autologous T-cell therapy, TAC01-HER2, in HER2-positive gastric and gastroesophageal junction cancers.
The firm began the potentially registrational Phase II portion of the TACTIC-2 study, which is evaluating TAC01-HER2 as a monotherapy and in combination with Merck’s Keytruda (pembrolizumab) in HER2-positive gastric cancers. Deyaa Adib, chief medical officer of Triumvira Immunologics, said in a statement that these tumor types were identified based on positive results from the Phase I portion of the study in solid tumors.